US Quiz of the Month – março 2025
Case Report
A 54-year-old male patient presented with postprandial bloating, progressive dysphagia and intermittent regurgitation over several months. There was no associated weight loss, anorexia, or chest pain. Physical examination was unremarkable, and laboratory tests revealed an elevated CA 19-9 level of 93 U/mL.
Computed tomography (CT) and magnetic resonance imaging (MRI) showed a large cystic lesion adjacent to the D2-D3 region of the duodenum. The origin of the lesion remained uncertain, leading to the decision for an endoscopic ultrasound (EUS) with fine-needle aspiration (FNA) for further characterization.
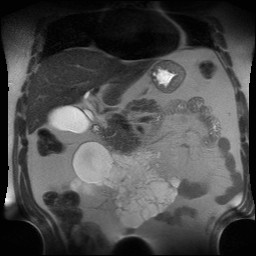
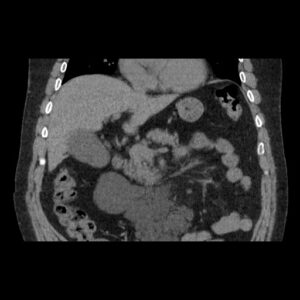
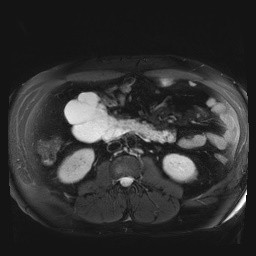
Figure 1 – MRI and CT images showing multiloculated cystic formation.
EUS was performed and a large multiloculated cystic formation was identified in the deep D2 region. The lesion extended beyond the field of study, preventing precise measurement. The largest cyst measured 28 mm, with multiple smaller cysts forming a “honeycomb” pattern. The cysts had thin walls and septations, without visible nodules, and their contents appeared anechoic and clear. No abnormal thickening was observed in the gastric cardia or other adjacent structures.
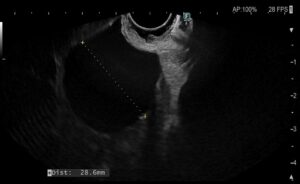
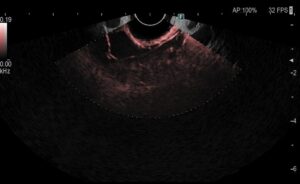
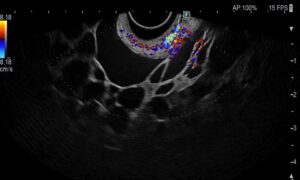
Figure 2 – EUS images showing multiloculated cystic formation.
FNA was performed using a 22G needle, aspirating fluid from two cysts and obtaining approximately 5 mL of milky fluid, which was sent for biochemical analysis. Additional samples from the septations were sent for cytopathological evaluation. The analysis revealed an extremely high triglyceride level (17324 mg/dL) and the cytopathological study did not reveal neoplastic cells.
What is the most likely diagnosis?
Discussion
Cystic lymphangiomas are rare benign malformations of the lymphatic system, most commonly found in the head and neck region of pediatric patients. However, intra-abdominal cystic lymphangiomas (ICL) can occur in adults, often presenting with nonspecific symptoms such as abdominal pain, early satiety, or dysphagia due to mass effect.
Histologically, these lesions consist of multiple cystic spaces lined by endothelial cells, often containing chylous fluid. The high triglyceride concentration in the aspirated fluid is a hallmark feature, aiding in diagnosis. Imaging studies, including CT, MRI, and EUS, are valuable for characterization, but definitive diagnosis requires cytopathological and biochemical analysis of aspirated fluid.
Complete surgical excision is the treatment of choice, as incomplete resection can lead to recurrence. In asymptomatic or minimally symptomatic patients, conservative management with surveillance may be considered.
In this case, the diagnosis was confirmed through biochemical and cytological analysis. Additional study with manometry was consistent with Type II Achalasia, supported by the findings in the esophageal transit, justifying the patient’s symptoms. Thus, the patient was proposed for myotomy. Regarding the lesion, given the absence of malignancy or symptoms, a multidisciplinary team recommended clinical follow-up and imaging surveillance.
References
- Kim BS, Sbar AD, Jatoi I. Intra-abdominal cystic lymphangioma. Surgery. 2000;128:834-5.
- Guinier D, Denue PO, Mantion GA. Intra-abdominal cystic lymphangioma: case report and review. Am J Surg. 2006;191:706-7.
- De Perrot M, Rostan O, Morel P, et al. Abdominal lymphangioma in adults and children. Br J Surg. 1998;85:395-7.
- Konen O, Rathaus V, Dlugy E, et al. Childhood abdominal cystic lymphangioma: imaging findings and differential diagnosis. Pediatr Radiol. 2002;32:88-94.
Authors
André Trigo1, Margarida Ferreira1, Pedro Narra Figueiredo1,2
1 Gastroenterology Department, Unidade Local de Saúde de Coimbra, Coimbra, Portugal.
2 Faculdade de Medicina da Universidade de Coimbra, Coimbra, Portugal.


